What signs of hiatal hernia after gastric sleeve? How to fix hiatal hernia after gastric sleeve? What causes hiatal hernia after gastric sleeve? What causes hiatal hernia after gastric sleeve symptoms? How to hiatal hernia repair after gastric sleeve? What are symptoms of hiatal hernia after gastric sleeve? Hiatal hernias and acid reflux disease disorder are not unusual place occurrences in overweight sufferers. There is a nearly linear correlation among BMI and GERD. Indeed, increased intraabdominal strain in obese sufferers stresses the sensitive phreno-esophageal membrane.
Weakness on this membrane ends in effacement of the attitude of His, laxity with inside the diaphragmatic crura, and migration of the intraabdominal esophagus into the chest. With time, a hiatal hernia develops, and acid reflux disease disorder worsens.
Hiatal Hernia After Gastric Sleeve is a topic that may interest people who have undergone gastric sleeve surgery, a type of weight loss surgery that involves removing a large portion of the stomach, leaving a small, banana-shaped pouch that can hold only a few ounces of food. This surgery helps people lose weight by limiting the amount of food they can eat and reducing the hunger hormone ghrelin.
However, gastric sleeve surgery may also increase the risk of developing a hiatal hernia, a condition where part of the stomach bulges through an opening in the diaphragm into the chest cavity. This can cause symptoms such as heartburn, acid reflux, chest pain, and difficulty swallowing.
Most overweight sufferers imparting for gastric sleeve surgical procedure be afflicted by GERD. Meticulous surgical approach is fundamental to obtain right hiatal hernia restore and a properly contoured gastric sleeve. When well performed, bariatric sufferers revel in a reflux unfastened weight reduction journey.
A hernia happens while there’s a weak point in a muscle wall -stomach or diaphragm, that lets in an organ to push via the weakened area. Obesity is a danger component for growing any hernia.
Hiatal hernias arise while the belly or intestines push via the diaphragm and into the chest cavity. Gastric sleeve sufferers can also additionally increase a brand new hiatal hernia or have worsening of pe-present small unrepaired hiatal hernia.
Hiatal hernia is a condition that occurs when a portion of the stomach protrudes through the diaphragm and into the chest cavity. While it can occur in individuals for various reasons, it has been observed that patients who have undergone gastric sleeve surgery may be at a higher risk for developing hiatal hernia.
A hiatal hernia can occur after undergoing a gastric sleeve surgery, and it is important to understand the potential risks and complications associated with this condition. A hiatal hernia is a medical condition where a portion of the stomach pushes up through the diaphragm and into the chest cavity. This can lead to symptoms such as heartburn, chest pain, difficulty swallowing, and acid reflux.
What is Hiatal hernia?
A Hiatal hernia is a displacement of a part of the stomach from where it should normally be, into the chest cavity. The most common type is a sliding type hernia. The junction of the esophagus and stomach of this type upward through the gaps in the diaphragm muscles.
Usually it gives no symptoms. In some patients, it can cause the development of reflux disease. In a less common para sophageal hernia, the esophagus – stomach junction is in its normal place, but the dome part of the stomach enters the chest cavity from the side of the esophagus.
In this second type of hernia, reflux disease does not develop, but it must necessarily be operated on, as there is a high probability of suffocation. A Hiatal hernia is a contraction of the upper side of our stomach towards the top of the large (diaphragm) that separates the abdominal and chest cavity.
Our esophagus passes through the small hole in the diaphragm before it merges with the stomach. In a Hiatal hernia, this hole widens and makes it easier for part of the stomach to pass into the chest cavity.
Small Stomach hernias are usually not a problem. For some other reason, if it does not matter by chance during the examination, you will not find out in any way. But with a large hernia of the stomach, food and stomach acid escape back into the esophagus, and the patient has serious complaints.
The diaphragm is a dome-shaped muscle that separates the chest cavity, which contains the heart and lungs, from the abdominal cavity, which contains the stomach, intestines, and other organs. The diaphragm helps with breathing by contracting and relaxing.
The esophagus is a tube that connects the mouth to the stomach, and passes through an opening in the diaphragm called the esophageal hiatus. The esophagus carries food and liquids from the mouth to the stomach.
A hiatal hernia is a condition where part of the stomach pushes through the esophageal hiatus and protrudes into the chest cavity. This can create a bulge in the lower part of the esophagus, and disrupt the normal junction between the esophagus and the stomach.
There are two main types of hiatal hernia:
- Sliding hiatal hernia. This is the most common type, and occurs when the upper part of the stomach and the lower part of the esophagus slide up and down through the esophageal hiatus. This type of hiatal hernia may not cause any symptoms, or may cause mild symptoms such as heartburn, belching, or regurgitation.
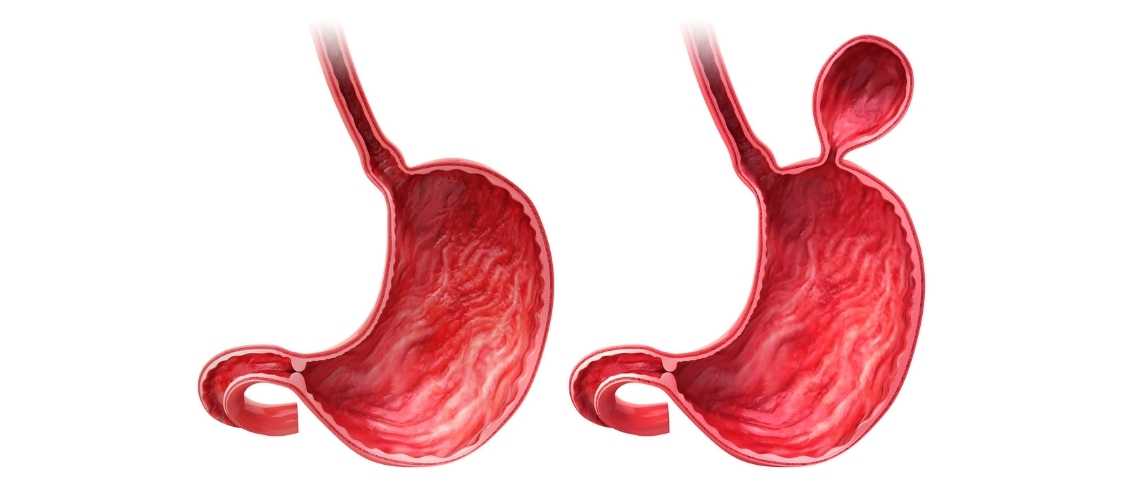
- Paraesophageal hiatal hernia. This is a less common but more serious type, and occurs when part of the stomach squeezes through the esophageal hiatus and stays there, next to the esophagus. This type of hiatal hernia can cause more severe symptoms, such as chest pain, difficulty swallowing, nausea, vomiting, or bleeding. It can also lead to complications, such as strangulation, obstruction, or perforation of the stomach.
Hiatal Hernia After Gastric Sleeve
What signs of hiatal hernia after gastric sleeve? Hiatal hernia is a condition that occurs when the upper part of the stomach bulges through the diaphragm and into the chest cavity. This can be a complication that arises after undergoing a gastric sleeve surgery, also known as sleeve gastrectomy.
Gastric sleeve surgery involves the removal of a large portion of the stomach, leaving behind a much smaller sleeve-shaped stomach. While this procedure is effective in promoting weight loss, it can also lead to an increased risk of developing hiatal hernias.
The connection between gastric sleeve surgery and hiatal hernias lies in the changes that occur in the stomach and the surrounding anatomy. The surgery alters the normal anatomy of the stomach and can result in the weakening of the diaphragm, which may allow the stomach to protrude into the chest cavity.
Symptoms of hiatal hernia after gastric sleeve surgery may include heartburn, chest pain, difficulty swallowing, and regurgitation. These symptoms can be uncomfortable and may affect the quality of life for individuals who experience them.
Treatment options for hiatal hernias after gastric sleeve surgery may include medication to reduce stomach acid, lifestyle modifications such as dietary changes and weight management, and in some cases, surgical intervention to repair the hernia.
It is important for individuals who have undergone gastric sleeve surgery to be aware of the potential risk of developing a hiatal hernia and to seek medical attention if they experience symptoms suggestive of this condition. Additionally, maintaining a healthy lifestyle and following post-operative guidelines provided by healthcare professionals can help reduce the risk of hiatal hernias and other potential complications following gastric sleeve surgery.
After a gastric sleeve surgery, which involves the removal of a large portion of the stomach to reduce its size and capacity, some patients may develop a hiatal hernia as a result of the changes in the anatomy of the stomach and the surrounding structures. The surgery involves removing a part of the stomach and reshaping the remaining portion into a smaller, sleeve-shaped tube. This alteration in the stomach’s anatomy can potentially lead to an increased risk of developing a hiatal hernia.
It is important for individuals who have undergone gastric sleeve surgery to be aware of the signs and symptoms of a hiatal hernia, as early detection and treatment can help prevent further complications. Some common symptoms of a hiatal hernia include heartburn, chest pain, difficulty swallowing, belching, and regurgitation of food or stomach acid. If these symptoms occur after gastric sleeve surgery, it is essential to consult with a healthcare professional for proper evaluation and management.
Diagnosing a hiatal hernia after gastric sleeve surgery typically involves a thorough medical history, physical examination, and imaging studies such as an upper gastrointestinal (GI) series or an endoscopy. These tests can help healthcare providers visualize the anatomy of the stomach and identify any abnormalities, including the presence of a hiatal hernia.
Treatment options for a hiatal hernia after gastric sleeve surgery may include lifestyle modifications, medications to reduce stomach acid production, and in some cases, surgical intervention. Lifestyle changes such as maintaining a healthy weight, avoiding trigger foods that can worsen symptoms, and elevating the head of the bed while sleeping can help alleviate symptoms associated with a hiatal hernia. Medications such as proton pump inhibitors (PPIs) or H2 blockers may be prescribed to reduce stomach acid production and relieve symptoms.
In cases where conservative measures are ineffective or if there are complications such as severe reflux or difficulty swallowing, surgical intervention may be necessary to repair the hiatal hernia. This can involve a procedure called a laparoscopic fundoplication, where the upper part of the stomach is wrapped around the lower esophagus to strengthen the valve between the esophagus and the stomach, thereby reducing acid reflux.
Symptoms of Hiatal Hernia After Gastric Sleeve Surgery
The symptoms of a hiatal hernia can vary from mild to severe and may include:
1. Heartburn: Individuals with a hiatal hernia may experience frequent heartburn, especially after consuming large meals or lying down.
2. Difficulty Swallowing: The protrusion of the stomach through the diaphragm can lead to difficulty swallowing, also known as dysphagia.
3. Chest Pain: Some individuals may experience chest pain or discomfort due to the herniated portion of the stomach pressing against the diaphragm.
4. Acid Reflux: The presence of a hiatal hernia can contribute to increased acid reflux, leading to regurgitation and a sour taste in the mouth.
5. Shortness of Breath: In severe cases, a hiatal hernia may cause difficulty breathing or shortness of breath, especially during physical activity.
It is important to note that not all individuals with a hiatal hernia will experience noticeable symptoms. Some hiatal hernias may be discovered incidentally during medical imaging or diagnostic tests for unrelated conditions.
Diagnostic tests for hiatal hernias may include:
1. Upper Endoscopy: This procedure involves the insertion of a thin, flexible tube with a camera (endoscope) through the mouth and into the esophagus and stomach to visually inspect the area and identify any abnormalities, including a hiatal hernia.
2. Barium Swallow: During this test, you will be asked to swallow a liquid containing barium, which will coat the esophagus and stomach, allowing for better visualization of any structural abnormalities on X-ray imaging.
Once a hiatal hernia has been diagnosed, your healthcare provider will discuss appropriate treatment options based on the severity of your symptoms and the impact on your overall health. Treatment for hiatal hernias after gastric sleeve surgery may include:
1. Lifestyle Modifications: Making changes to your diet, such as avoiding large meals and acidic or spicy foods, as well as maintaining a healthy weight, can help alleviate symptoms associated with a hiatal hernia.
2. Medications: Over-the-counter or prescription medications that reduce stomach acid production or neutralize acid reflux may be recommended to manage symptoms such as heartburn and acid reflux.
3. Surgical Intervention: In cases where lifestyle modifications and medications are ineffective in managing symptoms, surgical repair of the hiatal hernia may be considered. This can involve laparoscopic techniques to reposition the stomach and repair the opening in the diaphragm.
Symptoms of Hiatal hernia
Gastric sleeve surgery, also known as sleeve gastrectomy, is a popular and effective weight loss procedure that involves the removal of a large portion of the stomach, resulting in a smaller, sleeve-shaped stomach. While this surgery has been proven to help individuals achieve significant weight loss and improve obesity-related health conditions, there are potential risks and complications that can arise, including the development of a hiatal hernia.
- Heartburn
- Food and drink coming back into the mouth
- Backflow of stomach acid into the esophagus
- Difficulty swallowing
- Frequent and short breathing
- Bloody vomiting and black stools (indicating stomach bleeding)
- Bad breath
- Bloating
- Age-related weakening of the diaphragm
- Having had an injury, trauma or surgery to that area.
- Congenital wide hiatus.
- Continuous and high pressure on surrounding muscles (such as coughing, vomiting, straining, intense exercise and lifting heavy objects)
- Obesity
- Old age
Hiatal hernia Treatment
Classical methods of treatment do not work in patients with advanced gastric hernia with complaints of reflux, endoscopic applications do not give the desired result. In such cases, surgical treatment is resorted to as a final and permanent solution.
In surgical treatment, the herniated part of the stomach is performed and the necessary interventions are performed and the patient is restored to health. The size of the disease is the determining factor in the need for surgical treatment.
Some measures for diagnosing a hiatal hernia encompass the use of an endoscope, which lets in the health practitioner to view the chest internally. Also, a barium swallow can be ordered. The barium, called a “assessment medium,” makes abnormalities extra obvious on an x-ray.
Although maximum bariatric surgical operation sufferers will now no longer enjoy a hernia, it’s far nonetheless crucial to be aware of symptoms, have to they occur.
If a hernia is left untreated, it could come to be extra full-size over the years and could positioned extra stress on surrounding tissues. This will increase the chance of extra extreme scientific complications.
Basically, it is based on the narrowing of the aperture in the diaphragm by removing the stomach section that has escaped back into the chest cavity to the abdomen. In some cases, synthetic patches are placed on this area so that the hernia does not recur.
Operations are usually performed laparoscopically (closed). It takes about 1-2 hours or so. Patients usually stay in the hospital for 1-2 days. They can return to their normal lives within 1 week. During this process, patients are assigned a diet program that shows the transition from liquid to solid.
Hiatal Hernia Repair after Gastric Sleeve
For a few individuals, reflux signs might also additionally solve following weight reduction and with clinical management, along with the usage of antacids for gastric acid suppression. A hiatal hernia can purpose signs of GERD or can get worse them in folks that already skilled reflux.
During hiatal hernia restore, the belly is back into the belly cavity, and the disorder with inside the diaphragm across the esophagus is repaired.
This restore allows save you belly contents from sticking out returned into the chest cavity. Although hiatal hernia restore is a choice for sufferers with a gastric sleeve, conversion to RY gastric pass can also additionally want to be taken into consideration if signs are severe.
How to fix hiatal hernia after gastric sleeve?
How to fix hiatal hernia after gastric sleeve? Hiatal hernia is a condition where a part of the stomach pushes up through the diaphragm muscle. This can sometimes occur after gastric sleeve surgery, which is a procedure that reduces the size of the stomach. When a hiatal hernia develops after gastric sleeve surgery, it can cause symptoms such as heartburn, chest pain, difficulty swallowing, and regurgitation of food.
Fortunately, there are several ways to address a hiatal hernia after gastric sleeve surgery. In this article, we will discuss how to fix a hiatal hernia after gastric sleeve, including both non-surgical and surgical treatment options.
Hiatal Hernia Non-Surgical Treatment Options
1. Lifestyle Changes: Making certain lifestyle modifications can help alleviate the symptoms of a hiatal hernia. This includes avoiding large meals, eating slowly, maintaining a healthy weight, and avoiding trigger foods that can exacerbate acid reflux.
2. Medications: Over-the-counter antacids or prescription medications such as proton pump inhibitors (PPIs) can help reduce the production of stomach acid and alleviate symptoms associated with a hiatal hernia.
3. Elevating the Head of the Bed: Raising the head of the bed by 6 to 8 inches can help prevent stomach acid from refluxing into the esophagus while sleeping.
4. Weight Loss: For individuals who are overweight or obese, losing weight can help reduce the pressure on the stomach and minimize symptoms associated with a hiatal hernia.
Hiatal Hernia Surgical Treatment Options
If non-surgical interventions do not provide adequate relief, surgical intervention may be necessary to repair a hiatal hernia after gastric sleeve surgery. Some of the surgical options include:
1. Hiatal Hernia Repair: During this procedure, the surgeon will reposition the stomach back into the abdominal cavity and repair the opening in the diaphragm to prevent the stomach from sliding back up.
2. Conversion to Gastric Bypass: In some cases, converting a gastric sleeve to a gastric bypass procedure may be recommended to address a hiatal hernia. Gastric bypass surgery involves creating a small pouch from the stomach and reattaching it to the small intestine, which can help alleviate symptoms associated with a hiatal hernia.
3. Linx Procedure: The Linx procedure involves placing a small, flexible band of magnets around the esophagus to help prevent acid reflux. This can be an effective option for individuals with a hiatal hernia after gastric sleeve surgery.
It is important to consult with a healthcare professional to determine the most appropriate treatment option based on individual circumstances and medical history.
Hiatal Hernia Recovery and Post-Operative Care
Following surgical intervention for a hiatal hernia after gastric sleeve surgery, it is important to adhere to post-operative instructions provided by the healthcare team. This may include dietary modifications, activity restrictions, and taking prescribed medications as directed.
Recovery time can vary depending on the type of surgical procedure performed and individual healing capabilities. It is essential to attend follow-up appointments with the healthcare provider to monitor progress and address any concerns during the recovery period.
Hiatal Hernia Preventing Recurrence
After undergoing treatment for a hiatal hernia, there are steps that can be taken to reduce the risk of recurrence. This includes maintaining a healthy weight, practicing good posture, avoiding heavy lifting, and following any specific guidelines provided by the healthcare provider.
How Do You Know If You Have a Hernia After a Gastric Sleeve?
After a gastric sleeve operation, hernias are possible but uncommon. A bulge or lump in the abdomen, pain or discomfort in the affected area, and weakness or pressure in the abdomen are all signs of a hernia. It is crucial to get in touch with your surgeon for a diagnosis if you notice any of these signs or have any worries about a potential hernia.
Hiatal Hernias – Rare Or Common After Gastric Bypass Surgery?
Are hiatal hernias rare or common after gastric bypass surgery? The answer depends on your individual circumstances. While gastric bypass surgery is safe, the procedure has risks.
These risks are listed below. During the surgery, your surgeon will guide your stomach and lower esophagus back into your abdominal cavity. He may also stitch the stomach to the connective tissue in your abdomen. Afterwards, you will follow a strict diet program.
While many bariatric patients do not experience hernias after surgery, it is always better to be safe than sorry. Even if you don’t experience any immediate symptoms, a hiatal hernia can cause other medical problems, including gastro-esophageal reflux disease (GERD), which can lead to further complications.
Hiatal hernias are generally asymptomatic, but they can lead to severe consequences, such as esophageal cancer.
After the surgery, you may have chronic symptoms. These include post-prandial epigastric pain, dysphagia, and nausea or vomiting.
Depending on your individual circumstances, your doctor may recommend an upper endoscopy or diagnostic imaging to confirm the presence of a hiatal hernia. A hernia may also present as an obstruction in the bowel.
Hiatal hernias are not rare after gastric bypass surgery. The risk is high, but it is not uncommon for patients to have one following the procedure. A hernia is an uncomfortable side effect that may require additional surgery.
Fortunately, gastric bypass surgery is an option that can help you lose weight and improve your quality of life. You should discuss any risks with your surgeon before undergoing the surgery.
What Signs Of Hiatal Hernia After Gastric Sleeve?
What signs of hiatal hernia after gastric sleeve? After gastric sleeve surgery, the stomach is reduced in size, and this can potentially lead to an increase in pressure on the hiatus, the opening in the diaphragm through which the esophagus passes. This increased pressure can result in the stomach pushing through the hiatus, causing a hiatal hernia.
So, what are the signs of hiatal hernia after gastric sleeve surgery?
1. Heartburn: Patients may experience persistent heartburn, especially after consuming meals. This occurs as a result of stomach acid flowing back into the esophagus due to the herniated portion of the stomach.
2. Difficulty swallowing: A hiatal hernia can lead to narrowing of the esophagus, making it difficult for food and liquids to pass through.
3. Chest pain: Patients may experience chest pain or discomfort, which can be mistaken for symptoms of a heart attack.
4. Regurgitation: The herniated portion of the stomach can cause food and stomach acid to flow back into the esophagus, leading to regurgitation.
5. Shortness of breath: In some cases, a hiatal hernia can put pressure on the lungs, causing difficulty in breathing.
It is important to note that not all patients who have undergone gastric sleeve surgery will develop a hiatal hernia. However, those who experience persistent symptoms such as heartburn, difficulty swallowing, chest pain, regurgitation, or shortness of breath should seek medical attention.
Diagnosis of hiatal hernia after gastric sleeve surgery can be confirmed through imaging tests such as an upper gastrointestinal (GI) series, endoscopy, or a barium swallow. Treatment options may include medication to reduce stomach acid, lifestyle changes such as avoiding large meals or lying down after eating, and in severe cases, surgical intervention to repair the hernia.
Why Does a Hiatal Hernia Occur After Gastric Sleeve Surgery?
The exact cause of a hiatal hernia is not clear, but it may be related to several factors, such as:
- Weakness of the diaphragm. The diaphragm may become weak or damaged due to aging, injury, surgery, or congenital defects. This can make the esophageal hiatus larger or looser, and allow the stomach to slip through.
- Increased pressure in the abdomen. The abdomen may experience increased pressure due to obesity, pregnancy, constipation, coughing, sneezing, or straining. This can push the stomach upward and force it through the esophageal hiatus.
- Reduced pressure in the chest. The chest may experience reduced pressure due to smoking, asthma, or chronic lung diseases. This can create a suction effect that pulls the stomach upward and through the esophageal hiatus.
Gastric sleeve surgery may increase the risk of developing a hiatal hernia, or worsen an existing one, due to several reasons, such as:
- Dissection of the hiatal ligaments. During the surgery, the surgeon may need to cut or loosen some of the ligaments that attach the stomach to the diaphragm, such as the phrenogastric and the phrenoesophageal ligaments. This can weaken the support and stability of the stomach and the esophagus, and make them more prone to herniation.
- Tubular shape of the gastric sleeve. After the surgery, the stomach becomes a narrow tube or sleeve that can hold only a small amount of food. This can make the stomach more mobile and flexible, and less anchored to the surrounding structures. This can also make the stomach more susceptible to sliding or squeezing through the esophageal hiatus.
- Rapid weight loss after the surgery. After the surgery, the patient may experience significant weight loss, which can improve their health and quality of life. However, rapid weight loss may also lead to enlargement of the esophageal hiatus, as the fat tissue around it shrinks and the diaphragm relaxes. This can create more space for the stomach to herniate.
- Regaining of body weight after the surgery. Some patients may regain some of the weight they lost after the surgery, especially if they do not follow the dietary and lifestyle recommendations. This can increase the pressure in the abdomen and the stomach, and push the stomach through the esophageal hiatus. It can also dilate the gastric sleeve, and make it more likely to herniate.
How is a Hiatal Hernia Diagnosed and Treated After Gastric Sleeve Surgery?
A hiatal hernia may not cause any symptoms, or may cause mild to severe symptoms, depending on the type and size of the hernia, and the presence of complications. Some of the common symptoms of a hiatal hernia are:
- Heartburn or acid reflux, which is a burning sensation in the chest or throat, caused by the regurgitation of stomach acid into the esophagus
- Belching or burping, which is the release of gas from the stomach or esophagus
- Regurgitation or vomiting, which is the return of food or liquids from the stomach or esophagus to the mouth
- Chest pain or discomfort, which may be sharp, dull, or squeezing, and may radiate to the back, neck, or arm
- Difficulty swallowing or dysphagia, which is the feeling of food or liquids getting stuck in the throat or chest
- Nausea or loss of appetite, which is the feeling of sickness or lack of desire to eat
- Bloating or fullness, which is the feeling of pressure or tightness in the abdomen or chest
- Shortness of breath or dyspnea, which is the feeling of not being able to breathe enough or easily
- Palpitations or arrhythmias, which are abnormal or irregular heartbeats
A hiatal hernia can be diagnosed by several tests, such as:
- Upper gastrointestinal endoscopy. This is a procedure that involves inserting a flexible tube with a camera and a light through the mouth into the esophagus, stomach, and duodenum. This allows the doctor to see the inside of the digestive tract, and detect any abnormalities, such as a hiatal hernia, ulcers, inflammation, or bleeding. The doctor can also take biopsies or samples of tissue for further examination.
- Barium swallow study. This is a procedure that involves swallowing a liquid that contains barium, which is a contrast agent that makes the digestive tract visible on X-rays. The doctor can then take X-rays of the chest and abdomen, and see the outline of the esophagus, stomach, and duodenum. This can show the presence and size of a hiatal hernia, and how it affects the passage of food and liquids.
- Esophageal manometry. This is a procedure that involves inserting a thin tube with sensors through the nose into the esophagus. The tube measures the pressure and movement of the esophagus and the lower esophageal sphincter, which is the ring of muscle that prevents the reflux of stomach contents. This can show how well the esophagus and the sphincter function, and how they are affected by a hiatal hernia.
- pH monitoring. This is a procedure that involves attaching a small device to the lower part of the esophagus, either through the nose or the mouth, or implanting it under the skin. The device records the acidity or pH level of the esophagus for 24 to 48 hours, and transmits the data to a recorder that the patient wears. This can show how often and how severe the reflux of stomach acid is, and how it is related to a hiatal hernia.
A hiatal hernia can be treated by several methods, depending on the type and size of the hernia, the severity of the symptoms, and the presence of complications. Some of the common methods of treatment are:
- Medications. Some medications can help relieve the symptoms of a hiatal hernia, such as:
- Antacids. These are drugs that neutralize the stomach acid, and reduce the burning and pain caused by reflux. They can be taken as tablets, liquids, or chewables, and are available over-the-counter or by prescription. Some examples are calcium carbonate, magnesium hydroxide, and aluminum hydroxide.
- H2 blockers. These are drugs that reduce the production of stomach acid, and prevent or treat ulcers and inflammation caused by reflux. They can be taken as tablets, liquids, or injections, and are available over-the-counter or by prescription. Some examples are ranitidine, famotidine, and cimetidine.
- Proton pump inhibitors. These are drugs that block the enzyme that produces stomach acid, and heal the damage caused by reflux. They can be taken as tablets, capsules, or injections, and are available over-the-counter or by prescription.